Charlotte Fairbairn—A New Baby …with Complications
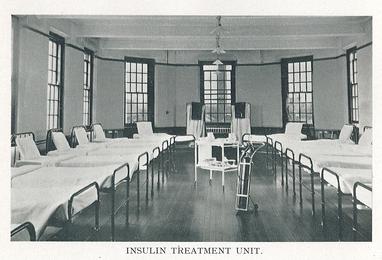
An insulin treatment ward, circa 1951 | Wikipedia
(Editor’s Note: I have selected some photos from Getty Photos and other sources that help illustrate scenes in the story, and may or may not be exactly representations of the people and places mentioned. For example, the above photo is that of a hospital in England from ~1951.)
This article is one of an 8-part series about Charlotte Fairbairn, and was written by our patron, John Fairbairn. To read the intro by the editor and see links to the other 7 parts of the story, refer to the Table of Contents page. On to the story—
Charlotte became pregnant in early March, and after a lengthy and difficult pregnancy, she bore her second son. On 13 December 1944, the couple welcomed John Lyndon Fairbairn. The delivering physician noted that the infant’s birth was breech and that the birthing process was extremely exhausting for the mother. At first, after overhearing a nurse speaking to her physician about an infant that died, Charlotte was convinced the new child was not hers and refused to nurse him. Three days of loving effort by Edward convinced her that the child was indeed a Fairbairn, through and through. Still, this had severe emotional and physical effects on Charlotte.
Three days of loving effort by Edward convinced her that the child was indeed a Fairbairn, through and through.
She remained in the hospital, with the doctor unwilling to discharge her and the new child until some sort of reliable rhythm and balance seemed to have been obtained. Charlotte recovered briefly, but then relapsed into physical exhaustion. The attending physician and the pediatrician agreed to take the infant from breast-feeding, and prescribed formula. That seemed to be Charlotte’s undoing. She was deprived of the stability of frequent intimate contact with her baby. This, and a biological upset to her endocrine system that often is caused by abrupt termination of breast feeding, made Charlotte enter the first of a number of sessions of mental agony. She was transferred to the University of Virginia Hospital and confined in the psychiatric ward there for three months. While there, she underwent a series of radical treatments in their new psycho-therapy section. This was insulin-shock therapy, in which the patient receives a huge dose of insulin that causes a massive depletion of blood glucose, with a resulting very rapid slide into diabetic coma.

Insulin shock therapy | Wikipedia
Origins of Insulin Coma Therapy
Insulin coma therapy was a form of psychiatric treatment wherein patients were injected repeatedly with large doses of insulin, in order to produce daily comas over periods ranging from several weeks to years. Introduced in 1933 by Polish-Austrian-American psychiatrist Manfred Sakel, it was used extensively in the 1940s and 1950s in the United States before being replaced by neuroleptic drugs.

Joseph Wortis, MD
Sakel made his results public in 1933 and his method soon was adopted by other psychiatrists. Joseph Wortis, after seeing Sakel practice it in 1935, introduced the concept into the USA. In 1936, Sakel moved to New York and also introduced insulin coma treatment into American psychiatric hospitals. By the late 1940s, the majority of psychiatric hospitals in the USA were using insulin coma as a standard treatment.
Technique
Insulin coma therapy (ICT) was a labor-intensive treatment that required trained staff and a special unit. Patients, who almost invariably were diagnosed with schizophrenia, were selected on the basis of having a good prognosis and the physical strength to withstand an arduous treatment. There were no standard guidelines for treatment; different hospitals and psychiatrists developed their own protocols. Typically, injections were administered six days a week for about two months. The daily insulin dose was gradually increased to 100-150 units until coma was produced, at which point the daily dose was leveled out.
Occasionally doses of up to 450 units were used. After about 50 or 60 comas, or earlier if the psychiatrist thought that maximum benefit had been achieved, the dose of insulin was rapidly reduced before that course of treatment stopped. Some courses lasted 2 years.
Many patients tossed, rolled, moaned, twitched, spasmed, or thrashed in response to random central nervous system impulses brought on by the deprivation of proper glucose levels.
After the insulin injection, patients experienced various symptoms of decreased blood glucose. These included: flushing, pallor, perspiration, salivation, drowsiness, or restlessness. If the dose was high enough, sopor (a deep, unnatural sleep) and coma followed. Each coma lasted for up to an hour and was terminated by intravenous injections of glucose. The basic concept was similar to the modern one of rebooting a computer: shut down the brain and let it restart. Seizures sometimes occurred before or during the coma. Some psychiatrists of the time regarded such seizures as therapeutic. Many patients tossed, rolled, moaned, twitched, spasmed, or thrashed in response to random central nervous system impulses brought on by the deprivation of proper glucose levels.
When they were not in a coma, insulin shock patients were kept together in a group and given special treatment and attention. One handbook for psychiatric nurses written by British psychiatrist Eric Cunningham Dax instructed nurses to take their insulin patients out walking and occupy them with games and competitions, flower-picking, reading maps, and the like. The hypoglycemia that resulted from ICT made the patients very restless, sweaty, and extremely likely to have further convulsions. Also, patients required continuous supervision as there was a danger of hypoglycemic (pathologically low glucose level) “after-shocks” after the coma. In addition, patients invariably emerged from the long course of treatment having gained considerable weight, often so much as to be termed “grossly obese”.
The most severe risks of insulin coma therapy were brain damage from prolonged coma, and death that resulted from an irreversible coma. A contemporary study claimed that many of the cases of brain damage actually were a therapeutic improvement, since the patients showed “a loss of tension and hostility”. In other words, to justify the continued practice of this treatment, and to excuse the resulting damage to conscious volition, some of the psychiatrists of the time claimed the treatment was a success even though the patient “partially died”. Mortality (death) risk estimates ran as high as 4.9 percent, a level that would be unacceptable in today’s psychiatric practice.
Effects
Sakel suggested the therapy worked by “causing an intensification of the tonus of the parasympathetic end of the autonomic nervous system, by blockading the nerve cell, and by strengthening the anabolic force which induces the restoration of the normal function of the nerve cell and the recovery of the patient.”
Although a few psychiatrists, including Sakel, claimed success rates for insulin coma therapy of over 80 percent in the treatment of schizophrenia, a few argued that it merely accelerated improvement in those patients who would undergo remission anyway.
The vast majority of belief at the time was somewhere in between. Most psychiatrists and physicians of the time claimed success rates of about 50 per cent in patients who had been ill for less than a year (about double the spontaneous remission rate), with no influence on relapse. Such claims were dubious, since no rigorous blind or double-blind testing was done until the mid-1950s. Sakel suggested the therapy worked by “causing an intensification of the tonus of the parasympathetic end of the autonomic nervous system, by blockading the nerve cell, and by strengthening the anabolic force which induces the restoration of the normal function of the nerve cell and the recovery of the patient.”
In layman’s terms, the shocks increased the constant low-level activity of a body tissue (usually applied to muscle tone, which has nothing at all to do with brain function) of that part of the autonomic (involuntary or subconscious) nervous system that counterbalances the action of the sympathetic nerves. It consists of nerves arising from the brain and the lower end of the spinal cord and supplying the internal organs, blood vessels, and glands. The sympathetic nervous system is a part of the nervous system that serves to accelerate the heart rate, constrict blood vessels, and raise blood pressure. The sympathetic nervous system and the parasympathetic nervous system constitute the autonomic nervous system. It did so, he stated, by somehow “blockading” these nerve cells, although exactly what he meant by this he never defined. Modern medications that “block’ the receptor sites of nerve cells were not developed until the late 1980s. Such medications did not exist in Sakel’s time. He also maintained that (somehow) this “strengthened” the chemical reactions that synthesize molecules in metabolism. Why he thought this non-psychiatric physiologic effect was useful in the treatment of psychoses remained undefined.
In other words, Sakel did not understand the physiologic function of nerve cells, or really have any idea exactly what (if anything) his experimental ‘therapy’ actually accomplished. Therefore, he spewed this pseudo-scientific gobbledygook as an explanation. Sadly, others in both his profession and the medical one bought this claptrap as an “enlightened” concept.
Decline
Insulin coma therapy was used in most hospitals in the United States during the 1940s and 1950s, but the numbers of patients treated were restricted by the requirement for intensive medical and nursing supervision, and the length of time it took to complete a course of treatment. In 1953 British psychiatrist Harold Bourne published a paper entitled The Insulin Myth in the British medical journal Lancet, in which he argued that there was no sound basis for believing that insulin coma therapy counteracted the schizophrenic process in any specific way. If treatment worked, he said, it was because patients were chosen for their good prognosis and were given special treatment: “Insulin patients tend to be an elite group sharing common privileges and perils”.
Unfortunately, this episode was only the first of a number of such deep depressive cycles for Charlotte. No one in that time understood the operation of the endocrine system and the effects of an off-kilter situation. Today’s treatment using tiny amounts of endocrine excretions, and indeed the ability to produce them, simply did not exist. She underwent several more bouts at the University of Virginia Hospital. During that time, a newer form of treatment – convulsive therapy – became increasingly popular because it did not require the large trained staff or time. As a result, combinations of the two therapies were tried until 1957. Patients sometimes were given cardiazol/metrazol convulsive therapy or electroconvulsive therapy during the insulin coma, or on the day of the week when they did not have an insulin treatment.
Many thousands of psychiatric patients already had suffered the traumas and indignities of this mentally excruciating treatment.
With the use of insulin coma treatment already declining, in 1957 Lancet published the results of a properly randomized, controlled trial where patients either were given insulin coma treatment or identical treatment but with unconsciousness produced by barbiturates. There was no difference in outcome between the groups. The authors concluded that, whatever the benefits of the coma regime might be, insulin was not a specific therapeutic agent. Meanwhile, in the United States, many thousands of psychiatric patients already had suffered the traumas and indignities of this mentally excruciating treatment. Sadly, many of those who survived it like Charlotte were compelled to do so again and again before the hospitals closed down their insulin shock wards.

Weston State Hospital
At that point, she became “unable to be treated effectively” at the University of Virginia Hospital. From then on, her manic-depressive cycles became the purview of the Weston State Hospital in Weston West Virginia. This ‘forward-thinking’ facility had been using electro-convulsive shock therapy for many years. Now began her real torment, the knowledge that when she next slid toward depression she would be remanded there unless she could afford therapy in a private facility. But, as she said, what was the use of that? All the psychiatric facilities, both public and private, had espoused this form of treatment with the same open arms they had extended to the earlier drug-shock ones. And, as later proper clinical trials would confirm, for the manic-depressive it was no more effective than had been the insulin-shock therapy.
Meanwhile, infant John languished in the hospital in Winchester. Edward, with the care and feeding of an active six-year-old to manage, plus a full-time job that was becoming increasingly difficult for him due to his own failing health, was unable to assume responsibility for the nearly around-the-clock requirements of tending a newborne. This situation must have been traumatizing for both of these parents.
Next week, Charlotte continues to recover from her mental ilness, and returns home. Despite the joy of a new baby, and the beautiful budding spring with warm weather and flowers, the Fairbairn family must weather through one more tragedy.
Link to “Home At Last …To More Tragedy” to be published October 10, 2017
Copyright Statement: Charlotte Fairbairn Story

